Malnutrition & Dehydration

Malnutrition
Nutrition is one of the most prolific topics related to pregnancy, yet when someone has HG, they are told malnutrition will not harm them or their unborn child. While surgical patients are typically given nutritional therapy within one week of being unable to eat, those with HG may go weeks or months nearly starving without nutritional intervention.
Women with HG may vomit or have severe nausea for months, leaving them exhausted, depleted and at risk for malnutrition and dehydration. It is imperative that women losing weight rapidly and not responding to medications be given nutritional support to prevent significant nutrient depletion in these women. Vitamins, especially B vitamins, are depleted quickly and if not replaced can worsen her symptoms or put her at risk for life-threatening neurological disorders like Wernicke's encephalopathy.
Vitamin Deficiencies
HG puts women and their babies are risk for malnutriton, including preventable vitamin deficiencies that can cause serious complications. Deficiencies left uncorrected may have numerous adverse effects on the breastfeeding child such as bleeding and neurodevelopmental disorders, especially if the mother had prolonged HG.
Vitamin B1/Thiamin Deficiency
Thiamin deficiency can lead to Wernicke's encephalopathy and heart issues.
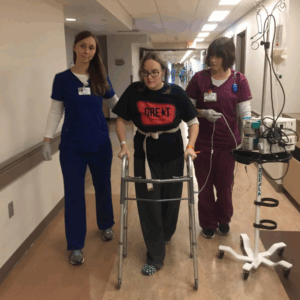
Alicia had to learn to walk again after developing Wernicke’s encephalopathy. Her most prominent difficulties were with thinking, speaking, and balance.
Vitamin K Deficiency
Vitamin K deficiency can lead to Binder's phenotype/embryopathy, resulting in abnormal fetal skeletal formation and abnormal clotting.
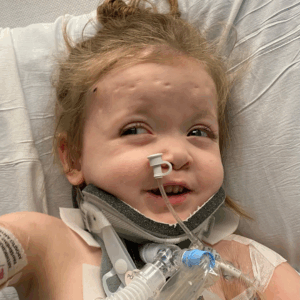
Addison was born with vitamin K embryopathy due to HG
Aggressive treatment is needed to promote a healthier outcomes and avoid preventable complications.
Fear of Malnutrition | Fear of Medication
One of the most difficult challenges with HG is managing nutritional needs. Every book, newspaper, magazine, and friend or family member will tell her repeatedly that she must eat healthy or she will harm her unborn child. The fear of harming her unborn child through lack of nutrition is closely followed by a fear of harming her unborn child with medications.
Dehydration
At a minimum, mothers requiring hydration should also receive vitamins and electrolytes. Those who continue to lose over 5-10% of their body weight in the early months should be considered for nutritional support to protect the well-being of both mother and child. These mothers are also at greater risk for complications such as pre-eclampsia, fetal loss, premature delivery, and more severe HG.
Studies show that an inadequately nourished fetus may grow and develop more slowly, have chronic disease in later life, experience emotional/behavioral and sensory issues, and more likely be preterm.
Swelling (Edema)
Edema may develop in some patients due to fluid shifts, low protein intake and refeeding syndrome. Monitor weight changes often until patients are asymptomatic and stable.
Additional Information
Need help?
If you find yourself asking, why am I vomiting more, or why aren’t my meds working? OR if you feel like you can’t go on, you may need IV fluids with vitamins.
Call your doctor if these persist or are severe or if you have a significant increase in breathing or heart rate.
Some choose termination (therapeutic abortion) rather than possibly face having a child who may have been harmed by malnutrition or medications.
Neurological Complications Due to Malnutrition
Neurological Conditions like Wernicke's Encephalopathy and Central Pontine Myelinolysis may be prevented in most cases by careful and proactive repletion of micronutrients. They may be fatal for the mother and unborn child if left untreated. Increasing numbers of cases are being reported each year. Symptoms differ in non-alcoholic patients like mothers with HG.
As we unravel the genetics of HG, we learn the same proteins that cause cachexia syndrome are involved in HG. The associated genes also alter appetite and taste perception making intake very difficult.
Kimber MacGibbon, RN
Our Case Study on HG and WE/CPM/EPM
Find recommendations on identification, prevention and treatment of Wernicke's encephalopathy.
WE is typically identified by the symptom triad of ataxia, confusion and oculomotor abnormalities. However, 10-47% of patients lack these signs, especially with ... non-alcoholic [HG] patients... Persistent or prolonged vomiting, confusion, and unintentional weight loss are red flags indicating a high risk of WE. Additional WE signs ... include weakness, dysarthria, confabulation, akinetic mutism, aphasia, cardiac failure, seizures, abdominal pain and nausea. Mental status changes are nearly universal and exhibited as dizziness, drowsiness, apathy, and cognitive impairment. Gait abnormalities range from weakness to inability to stand...
MacGibbon K, Fejzo M, Mullin P. Mortality Secondary to Hyperemesis Gravidarum: A Case Report. Women’s Health & Gynecology. 2015;1(2):011.